The number of deaths caused by coronavirus continues to rise, but are people without COVID-19 dying because of the lockdown?
Mental health issues, a reluctance to ask for medical assistance, and not wanting to add more pressure on the health services could be reasons why people are not accessing the help they need.
Could there be an increase in the number of people taking their own lives?
Tom Dening, professor of dementia research, faculty of medicine and health sciences at the University of Nottingham, said: “There doesn’t seem to be any data that so far suggests there is a wave of suicides.
“It is however quite possible that we will see an increase in suicides and self-harm over time, the longer the lockdown goes on.”
Read more about mental health:
- Can we stop male suicide?
- Lockdown: why is social isolation so hard?
- Can baking improve your mental health?
While Dr Dean Burnett, honorary research associate at Cardiff Psychology School, said the measures may be pushing people to their limits.
He said: “Most anxiety is caused by perhaps imagined threats and concerns, or potential dangers which may be, whereas now in the news they are telling us every day that there’s a genuine risk, just by leaving your house.”
He added that the feedback loop could lead to things becoming “intolerable” and could be when “things like suicide occur”.
- Subscribeto theScience Focus Podcaston these services:Acast,iTunes,Stitcher,RSS,Overcast
- If you have been affected by the themes discussed in this podcast, you can find support and information at samaritans.org. Samaritans is a safe place for anyone to talk about difficult feelings, 24 hours a day. Those in the UK and Ireland can phone free on 116 123.
Do people still feel able to attend hospital?
Prof Dening said there could be a number of reasons for what appears to be a sharp increase in deaths in the community that are not known to be due to COVID-19.
He explained: “These include people not feeling able to attend their GP surgeries, call an ambulance or attend A&E as they may have done in the past.
“Therefore, some serious conditions may present too late for effective treatment.
“Concern has been expressed by doctors working in children’s emergency care that they are not currently seeing the usual range of childhood emergencies.”
Linda Bauld, professor of public health at the University of Edinburgh, said some people have not been able to get appointments, or are told to arrange a virtual GP appointment and think “I am not going to bother”.

What are people with potentially fatal conditions doing?
Prof Dening said: “Another possibility is that some people with serious conditions, like cancer or chronic kidney disease, are either unable or unwilling to attend hospital on the usual regular basis, so their treatment regimes may lapse.
“Managing conditions like unstable diabetes will be much harder remotely than with face-to-face attention.
“Or there may be people who would have been referred to specialists for assessment of potentially serious conditions, where there is now a delay in offering appointments or indeed clinics may simply have been cancelled.”
Prof Bauld explained that some people may have had a procedure that they need delayed, resulting in unintended consequences.
Could the lockdown lifestyle itself be harming health?
Prof Dening said the lockdown itself may be breeding unhealthy behaviour.
He told PA: “Some people confined to their homes are likely to be drinking and smoking more, or eating less healthily, and this may also contribute to health problems, including accidents, around the home.”
How to stay safe during lockdown:
- Coronavirus: Is hand-washing really the best thing we can do to stop the spread of COVID-19?
- Should we all wear face masks?
- Which science and tech shows to stream, watch and listen to during lockdown
- 10 science-backed tips to help you work from home successfully
What do the numbers say about the deaths?
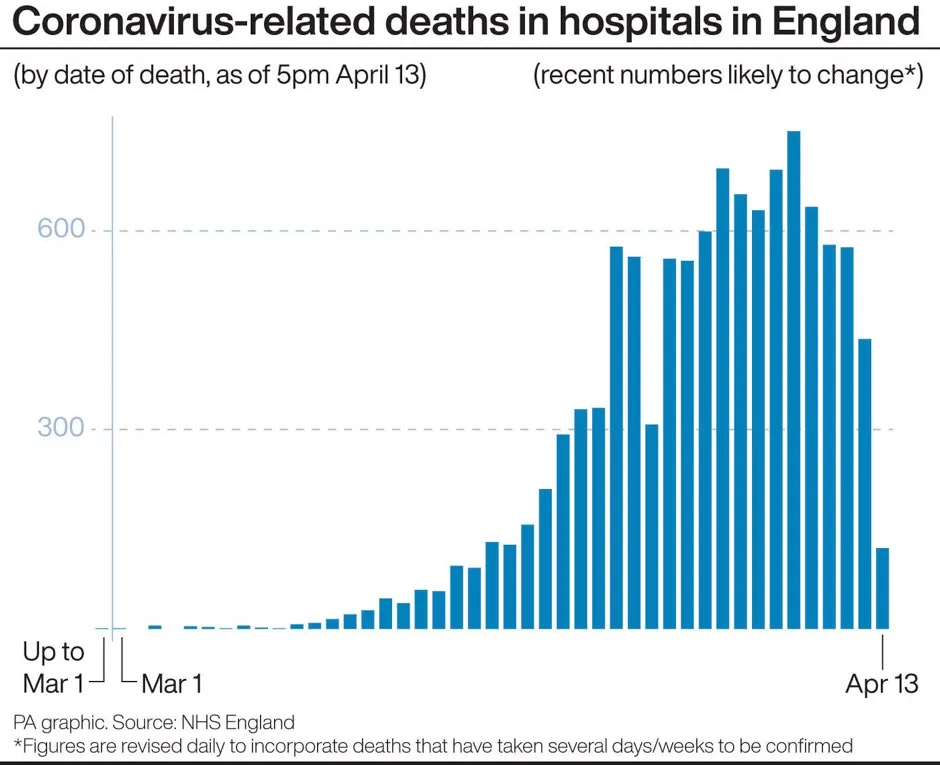
Of the 16,387 deaths registered in England and Wales during the week ending 3 April, around a fifth (3,475) mentioned “novel coronavirus”.
But the ONS said there were 6,082 more deaths during that week compared to the five-year average, which raises questions about the reasons behind the remaining two and a half thousand additional deaths.

Professor Maureen Baker, former Chair of the Royal College of General Practitioners (RCGP), said there could be a number of explanations.
“Data from previous pandemics of the 20th Century have shown that health pandemics tend to lead to a rise in all-cause mortality,” she added.
“There could be greater difficulty for people with non-COVID symptoms to currently get access to hospital services, or not wanting to access them due to the COVID risk.
“It might be the case that people with emergency symptoms – for instance, chest pain, abdominal pain, severe headache – are not consulting a doctor as early as they normally would with such symptoms.”
