Back in January, when the coronavirus was very new and was still confined to Wuhan, we were working on the assumption that COVID-19 was more or less an ordinary respiratory disease. The WHO described the symptoms as “mainly fever, with a few cases having difficulty in breathing,” with some patients developing pneumonia.
Even on 31 January when the UK’s first cases were confirmed, Chief Medical Officer for England Professor Chris Whitty described COVID-19 as a “relatively minor disease” for most people, going on to say that those who were most seriously affected would be treated “as anyone else with a respiratory disease.”
As time went on, however, more and more symptoms have been added to the list. “People have a very large number of different symptoms and many of those symptoms aren't immediately obviously related to infection,” says Ajay Shah, professor of cardiology at King’s College London. “People with diarrhoea. People come in with confusion. People come in with chest pain.”
Read the latest coronavirus news:
- COVID-19: Outcome 'not good' in UK, says chief scientific adviser
- Isle of Wight COVID-19 cases 'rapidly declined' after test and trace launch
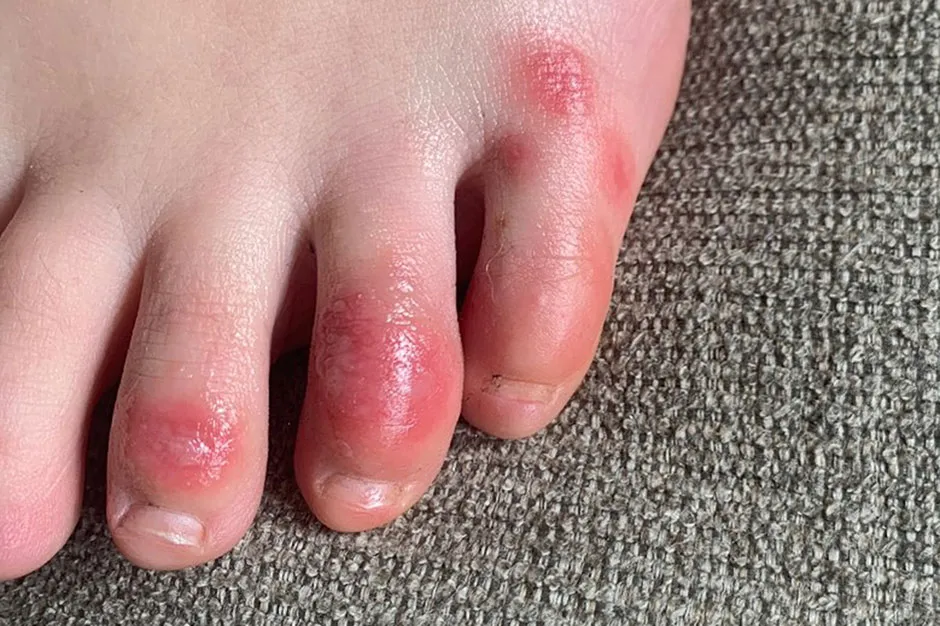
The list goes on. Some patients report rashes like ‘COVID toe’, which appears on the feet. And even if the cough and fever clear up, patients can end up suffering a heart attack, stroke, or kidney failure. In fact, one study found that heart problems played a role in 40 per cent of COVID-19 deaths.
So how could a flu-like illness cause all of these different symptoms?
“I guess the starting point is it's definitely not a simple infection,” says Shah. “You might think maybe people who've had chest problems are more likely to get [severe COVID-19], like COPD or asthma. But actually, you are much more likely to get nasty COVID if you have pre-existing cardiovascular conditions.”
It turns out that COVID-19 affects the endothelium, which is the layer of cells that lines the inside of blood vessels, as described in a paper published in The Lancet, hinting at how COVID-19 could affect the entire body. “The virus actually uses a particular receptor on the endothelial cells,” says Dr Nicola Mutch, a molecular biologist at the University of Aberdeen.
Once it’s attached to this receptor, SARS-CoV-2 (the virus that causes COVID-19) finds its way inside the endothelial cell, and from there, causes a huge inflammatory immune response called a ‘cytokine storm’. “All of us need to have an inflammatory response to tackle an infection. But for most of us, it's properly tuned,” says Shah.
While it’s not yet clear why the immune response differs from patient to patient, and overactive inflammation response causes more problems than it solves, potentially leading to organ failure and even death. “It seems that in people with COVID, this is a very, very important part of why people end up needing hospital,” he adds.
Shah believes that the progression of severe COVID-19 can be broken down into stages. The first one is this exaggerated inflammation, the cytokine storm. The second is a problem with blood clotting, known as coagulopathy.
“Very early on when we started seeing the patients, we noticed that a lot of patients were developing clots everywhere,” Shah explains. “Getting clots in the lungs. Some patients are getting clots in their hearts. Some people are getting clots in the brain.”
A study published in Thrombosis Research confirmed that blood clots were linked to an increased risk of death in COVID-19 patients.
This could easily explain many of the complications of COVID-19. “If you have this kind of systemic coagulopathy, systemic problem with clotting, then it's very easy to imagine how the disease kind of goes out of control and begins to affect lots of different parts of the body.” Strokes and organ failure, for example, can both happen as a direct result of a clot preventing blood flow.
Read more from Reality Check:
Luckily, this means we already have plenty of ready-made treatments that can be applied to COVID-19. “We're fortunate that we do have a number of anti-coagulant drugs that have previously had some success,” says Mutch. “We're always looking for new anti-coagulant drugs, to be honest.”
We could even go back a step and treat the inflammation. “Treating the inflammatory response to stop the thrombosis is also another possibility,” Mutch explains. The low-cost steroid dexamethasone, is one possible treatment: in June, it was shown to reduce deaths among patients on ventilators by up to a third.
“I think the most possibly the most important take home message would be that it's a very complicated disease, which is not the same in everybody,” says Shah. “We probably need to look much more carefully at the individual patient and then decide what's the best treatment for that particular patient.”
Visit the BBC's Reality Check website at bit.ly/reality_check_ or follow them on Twitter@BBCRealityCheck

