A study carried out at the National Hospital for Neurology and Neurosurgery, UCLH, on a small number of confirmed or suspected COVID-19 patients has linked the coronavirus to a number of neurological conditions, including delirium, stroke and brain inflammation.
Dr Rachel Brown, one of the study's authors, is an MRC Clinical Research Training Fellow affiliated to the UCL Queen Square Institute of Neurology and the UCL Institute of Immunity and Transplantation. We asked her why COVID-19 might be connected to the brain.
COVID-19 is primarily thought of as attacking the respiratory system but your research shows it can lead to the development of neurological syndromes.
COVID-19 is still predominantly a respiratory illness, but in a small subset of patients, we’ve been seeing neurological symptoms and syndromes. Some of the early studies from Wuhan showed that around a third of patients were having neurological symptoms.
In those early descriptions a lot of the symptoms that people were describing included things like headache and dizziness, loss of smell and things that could just really be attributed to viral illness. But as we gained more experience, we noticed other cases appearing that looked a little bit different.
Read more about the effects of COVID-19:
- Coronavirus: 'Concerning increase' in rare brain inflammation
- COVID-19: Have we been treating the disease wrong?
We have previous information from other viral illnesses, SARS and MERS and things like that in the past, so it wasn’t unexpected that neurological symptoms or syndromes might come out of COVID-19 as well.
At our centre, which is a specialist neuroscience centre linked with lots of different hospitals and centres across London and the UK, we already had a multidisciplinary platform for discussing inflammatory and infectious diseases. When COVID-19 came we set up a weekly meeting open to colleagues across London.
By doing that we were able to pool experience as it was coming through. That was really important, that collaborative effort, because these complications are on the rare end of the spectrum. It allowed us to spot patterns in what we were seeing.
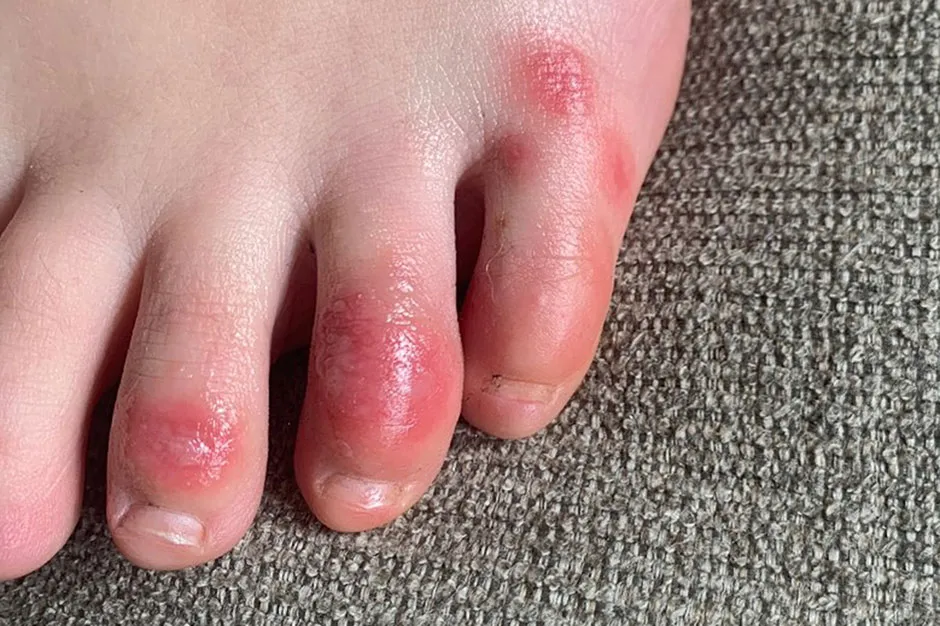
The sorts of things we were seeing were encephalopathy, which is a transient brain dysfunction, a delirium-type condition, which can be very common in infections and with hospital admission generally, and we were also seeing patients with post infectious problems with the brain or the nerves - this ADEM-like (acute disseminated encephalomyelitis) illness and also some patients who had Guillain-Barré syndrome as well.
We were also seeing some unusual strokes. We now know that COVID-19 can make your blood very sticky and in some patients, that can lead to development of stroke, even in those where there aren’t traditional risk factors.
What are the effects of ADEM and Guillain-Barré syndrome?
They’re both what we call para- or post-infectious inflammatory syndromes affecting the nervous system, that is, inflammatory syndromes that arise in the context of or after infection.
ADEM affects the brain and the spinal cord, usually after an infection, and is actually usually most common in children and adolescents. About half of them have an antibody against one of the proteins on the myelin sheath – the protective sheath around the nerves in the brain. Patients can be very unwell.
They can get headaches, they can be drowsy, they can have weakness, sometimes seizures. But it tends to be a one-off illness with recovery afterwards.
Guillain-Barré is similar in that it’s also a post-infectious inflammatory syndrome, but it affects the peripheral nerves supplying movement and sensation to the arms and legs. It’s thought to be an immune cross-reaction, where the immune system that’s trying to fight off the virus mistakes certain proteins or cells in our body for those viruses and then can lead to inflammation.
How common are these neurological complications likely to be?
I would stress that on the whole I think the neurological complications are likely to be rare, and that the complications we are describing are on the more severe end of the spectrum.
We wouldn’t want to cause alarm with this paper. Our paper and probably other surveillance type studies are going to bias towards the more severe end because we’re tending to see the patients who are presenting to hospital.
When these complications do happen, they can be very severe and can be life-changing, so it is important that we know about them, but on the whole they are likely to be rare.
Read more coronavirus news:
- COVID-19 'more severe' in cold weather, study suggests
- COVID-19 vaccine trials in China deemed safe to move to phase three
Is it possible that the patients had pre-existing conditions that the virus then exacerbated?
The neurological symptoms were largely new things. It’s possible that certain underlying health conditions might make people more prone to things like stroke or encephalopathy.
We know that encephalopathy is common in patients who have febrile illnesses [fever], particularly with advancing age, so there’s probably some sort of underlying factors there.
So it’s not so much an exacerbation of things that were already there, but maybe that there are some certain predisposing factors that make people a bit more prone, but we don’t really know what they are yet.
Are there any treatments that we could use to lower the risk of these neurological complications from emerging in patients who are hospitalised with COVID?
What we don’t know at the moment is exactly what is driving each of these conditions. We know that ADEM and Guillain-Barré are usually post- or para-infectious auto inflammatory illnesses, but some of the cases were a little bit more unusual.
We described some of the ADEM cases as ADEM-like and saw small areas of microhaemorrhage (bleeding) more than we would expect. The delirium cases could have a range of underlying causes.
For the stroke cases, the prothrombotic [causing blood clotting] effect that COVID-19 can trigger may be having an effect. There are probably a number of different mechanisms underlying the different neurological syndromes that we’re seeing, some of which we suggested in the paper.
One thought is whether the virus itself is doing some of this, but we don’t actually have a lot of good evidence, and very few reports have actually found the virus in the brain or in the spinal fluid. So that’s either related to the way we were looking for the virus or testing for it, maybe our tests aren’t sensitive enough, or maybe it’s actually that there are other things that are underlying these conditions.
The immune system is probably going to be a major factor for a number of these complications, but there also might be other factors. For example, some patients can become very hypoxic, that’s low oxygen levels, we know that that can affect the brain and the nerves, and for others there may be a contributory effect of a prolonged or severe illness, including admission to the ICU.
What are the next steps for this research?
I think what’s been really exciting is just how much the medical community has mobilised and come together. The sorts of things that my colleagues across the UK and across the world will be doing will be to try to understand each of these conditions better, to find out exactly what is driving each one.
We need to look at each category. We need to see how frequently this is actually occurring and how many people it’s affecting.
Is it the virus itself or the illness that is triggering it? What are the underlying mechanisms?
We need to identify which patients are most at risk so that we can try and reduce the risk of these neurological complications happening and then we need to look at how we’re going to treat each one.