Though still in the midst of the current COVID-19 pandemic, we are now seeing warning signs of another disease popping up in countries around the world - monkeypox. This is not a new virus (it was first discovered in 1958), nor is the virus new to the UK (there have been regular small outbreaks over the years). However, we are now seeing wider spread of the virus, with 100 cases and nearly 300 suspected cases reported in more than 16 countries, including 57 cases in the UK, as of 24 May. Are we staring down the barrel of yet another disease pandemic?
Recent years have seen 13 isolated outbreaks of monkeypox that have been mostly contained to a single country and can be traced back to travel from Central and West Africa, where the virus is thought to reside. In May and June 2021 there were three cases of monkeypox in the UK that were linked to recent travel to West Africa. However, according to the World Health Organization, the current outbreak is proceeding differently, with many more cases, more human-to-human transmission and more people that were infected outside of Africa.
In Central and West Africa, monkeypox typically spreads from infected animals to humans (or monkeys, hence its name), though some human-to-human transmission does occur. The Centre for Disease Control and Prevention states that monkeypox infections first result in fever, headache, fatigue and swollen lymph nodes, followed by a rash that develops into blisters (pox) on the skin - including in the mouth, on the genitals, eyes or the soles of the feet.
Monkeypox infections usually develop 1 to 3 weeks after exposure, with infections lasting 2 to 4 weeks. Most infections are relatively mild, though the blisters can be quite painful. However, depending on the specific strain of monkeypox, the infections can be fatal in up to 10 per cent of the cases, though the current outbreak has a lower fatality rate of around 1 per cent.
There are several therapeutics developed for smallpox that should work on monkeypox, and several effective vaccines are available for high-risk individuals. In addition, a study carried out in the 80s at the London School of Tropical Medicine and Hygiene found that previous smallpox vaccination can help to protect against monkeypox, though routine vaccination against smallpox was ended in the UK in 1971, and so the overall immunity has been declining year on year.
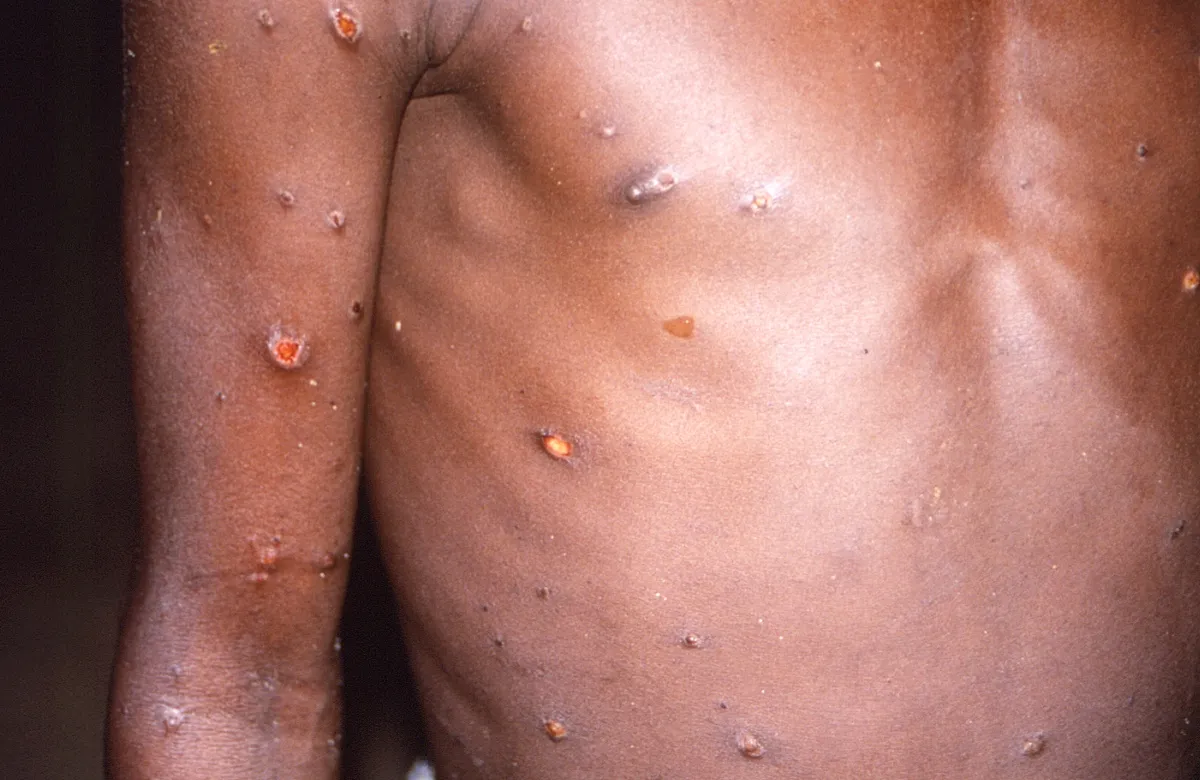
During a case of monkeypox, the rash and blisters can be highly infectious, typically through close contact between people. In some cases the virus may spread through the air, though a study led by researchers in Geneva suggests it is far less infectious than COVID-19. Regardless of the type of transmission, isolation of individuals with rashes or blisters is highly effective at preventing monkeypox transmission.
The question on everyone’s mind is why is this current monkeypox outbreak so different from previous ones and how worried should we all be? The short answer is that we don’t yet know why this outbreak is different from all the rest.
It’s possible that the recent return to travel and large social gatherings following relaxation of COVID-19 restrictions has resulted in more cases of monkeypox transmission in a short period of time. It is also possible that the virus has changed or mutated in some way that is enabling more virus transmission, though current data suggests that this strain of the virus is very similar to the West African strain that has previously caused small outbreaks.
Alternatively, this outbreak may be progressing differently due to previous COVID-19 infections. We know that COVID-19 infections can cause dysregulation of our immune system and recent evidence from a study by Australian researchers suggests that this dysregulation may persist for weeks-to-months following infection, even in people without persistent symptoms (i.e. long COVID).
It is possible that this immune dysregulation increases susceptibility to infection, facilitates virus transmission or alters the clinical disease. If this is the case, and it is far from proven, then we may see more unusual infectious disease outbreaks in the coming months.
Regardless of the reason for the unusual nature of the current monkeypox outbreak, it is likely that we will see more cases over the coming weeks. As people can take up to three weeks to become symptomatic and can spread the virus for up to a month, it will take some time before we know the full size and scale of this outbreak. Given that monkeypox mainly spreads through close contact with someone that has the rash or blisters, it is unlikely that this outbreak will become a new epidemic or pandemic.
However, there are risks to individual people and it is important to be aware and cautious. Talk to your doctor if you notice any rashes or blisters/pox and be cautious before coming into close contact with others. As with COVID-19, remember that misinformation is widely spread and to be cautious of what you read on social media. Refer instead to trusted sources such as the NHS.
This is a new and rapidly changing outbreak and the information may change quickly, so stay up to date and remember that the COVID-19 pandemic is still going on, with new immunity-evading variants and a continued need for precautions. Thankfully, the measures that stop the spread of COVID-19 will also stop the spread of monkeypox.
Read more about viruses:
