Can you keep your eyes open long enough to read this feature? We won’t be offended if you can’t. The Royal College of Psychiatrists says that one in five of us feels unusually tired at any one time, and one in ten feels permanently fatigued. Tiredness and fatigue are behind 20 per cent of UK doctor consultations, according to a recent survey of GPs. No wonder doctors are regularly jotting down a handy new acronym – TATT (Tired All The Time) – in patient notes. Or that UK sales of energy drinks shot up by 155 per cent between 2006 and 2014. We are, it seems, an exhausted nation.
Tiredness is no joke. Sleep deprivation brings a heavy mental and physical toll. Around 20 per cent of accidents on major roads are sleep-related, according to the Department of Transport. Plus, people who are sleep-deprived lose the ability to be positive-minded, whichresearchers from the University of Pennsylvania say is likely to increase the likelihood of depression. There’s also evidence that sleep deprivation increases the risk of obesity, heart disease, diabetes and stroke.
Even if you’re getting enough sleep, feeling constantly fatigued can be bad for you. Research from the University of Alabama has found that working hard while fatigued increases blood pressure. This is because tired people increase their effort to make up for their diminished capability when they want to accomplish a task.
For those with conditions such as chronic fatigue syndrome (CFS/ME) and cancer, it severely restricts quality of life. For millionsof others, unexplained tiredness regularly rumbles in the background. Is theresomething wrong with us? Are we the victims of hectic 24-hour lifestyles? Why are we tired all the time?
Until now, little has been known about the biological processes that result in what we call tiredness or fatigue. Only in recent decades, with growing concern about the prevalence of conditions such as CFS/ME, has researchmoney been invested into the causes of long-term fatigue. And it is becoming clear that, although there is a wide spectrum of tiredness types, they are all linked and their causes interact.
Prof Julia Newton, director of the Newcastle Centre for Fatigue Research at Newcastle University, explains the causes of tiredness via a classic bell-shaped curve graph. “At the thin end of the curve, there are people who just need to get some sleep and get their lifestyle in order. At the other thin end of the curve there are clearly people who have diagnosed or undiagnosed illness that is causing fatigue. And then, there’s everything else in the wide middle part of curve.”
The wide middle is the complex bit, covering tiredness caused by combinations of many environmental, lifestyle and health factors. And recent research is beginning to reveal how genetics, cell function, inflammation and the brain’s response to light may all have an underlying role in this tiredness ‘mainstream’.
Tired bodies
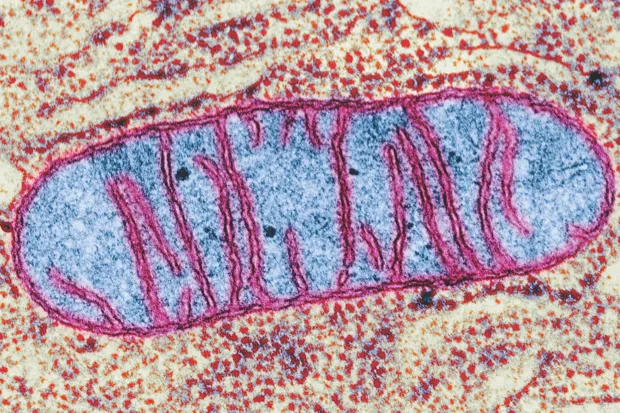
At a cellular level, scientists are increasingly looking at the role of mitochondria – the power packs in every humancell – in determining how tired we feel. Mitochondria are miniature organs (organelles) that convert oxygen, sugar, fats and protein into a form of chemical energy, called ATP, which the body uses to fuel the brain and muscles. Diseases affecting the mitochondria cause fatigue, so recent reviews of research suggest that fatigue is closely associated with mitochondria not working properly because the body is not producing particular enzymes, for example.
Studies into CFS/ME by American fatigue expert Dr Robert Naviaux have shown that the condition is characterised by changes in mitochondria function. Naviaux believes that these changes may be triggered by stressors such as infection, or physical and psychological trauma.
Naviaux cites new literature indicating that stress can prompt metabolic changes which make organisms go into hibernation-like states such as torpor, diapause and aestivation. “Each of these is an energy conservation state that permits survival under conditions of environmental stress at the expense of a decrease in the ability to allocate energy for daily work or activity,” he says. “Mitochondria are central control points for each of these processes.”
Are you sleep-deprived or fatigued?
Researchers use a simple sleep latency test to find out whether people who are constantly tired are sleep-deprived or fatigued for other reasons. If you lie down somewhere quiet during the day and fall asleep within a few minutes, then you are either lacking sleep or potentially suffering from a sleep disorder. If you don’t drop off within 15 minutes, fatigue is the problem.
This exploratory research about the metabolic origins of fatigue may link with other studies suggesting that sometimes tiredness has underlying but undiscovered physical origins. For example, recent studies have indicated that severe fatigue is associated with raised levels of leptin, a hormone produced in fat tissue which signals to the brain that the body has adequate energy stores. This raises the prospect that too much leptin – possibly from too much body fat – means we naturally feel less energetic: if we don’t need food we don’t need to go out and do something about it. This links with anecdotal evidence that intermittent fasting and reducing body fat can improve people’s energy levels.
It also links with research indicating that people with CFS/ME can have high levels of leptin and similar inflammation-producing substances called cytokines. Cytokines, which are also produced in fat, are released during immune responses. Studies have shown that low-grade inflammation robs mice of their energy to run on a wheel. This suggests that underlying tissue inflammation – whether it’s in response to a virus, a long-term condition or a problem with cytokine regulation – can be enough to make us feel weary. Scientists in the Netherlands have now started a major new trial to find out whether anakinra, an anti-inflammatory drug that blocks a particular cytokine, brings an improvement in people with CFS/ME.
Newton is clear that these related underlying physical vulnerabilities may be a factor in everyone’s continuing tiredness – not just those with a diagnosed condition. “The day-to-day fatigue that GPs see definitely relates to chronic illness. The two aren’t separate,” she says.
Naturally sleepy
There’s new research to suggest some of us may simply have been born with a physical and psychological susceptibility to tiredness.
Researchers from the University of Edinburgh analysed the genetic make-up of 111,749 people who indicated they felt tired in the two weeks before samples were collected for the UK Biobank. They found a genetic link between those who reported tiredness and those prone to diabetes, schizophrenia, high cholesterol or obesity. “This raises the possibility of a genetic link between tiredness and vulnerability to physiological stress,” said the team, led by Prof Ian Deary. However, the researchers also said that the majority of people’s differences in self-reportedtiredness can be put down to environmental causes rather than genetic factors. So how we live our lives, and what happens to us, is of first importance.
And the significance of our relationship to daylight is becoming increasingly clear. For decades, we’ve been told that keeping regular habits and sleeping hours is important. Now, research has confirmed the importance of a part of the brain called the suprachiasmatic nucleus (SCN), a group of cells in the hypothalamus that responds to light signals fed from the eye. When it’s light, the SCN messages other parts of the brain to release hormones which make us feel alert, and when it’s dark it signals for the release of hormones that make us feel sleepy, like melatonin.
If our habits are regular, our brain adjusts to release hormones at the right time. If they’re not, we end up in constant conflict with our natural circadian rhythm. The blue imitation daylight emitted from computer screens and smartphones can confuse our SCN further, especially if we’re using our screens at night. Our brain is tricked into thinking it’s day when it’s not, and we end up feeling awake when we should be sleepy, so we don’t get such a good night’s rest.
There’s increasing public and scientific interest in using what are known as ‘chronobiotic agents’ to adjust the body clock to counter sleep problems, tiredness and mood disorders. Studies investigating whether taking melatonin tablets reduces fatigue have been mixed, and doctors warn against overuse of the supplement. But some new types of antidepressants, such agomelatine, work by regulating circadian rhythms and there’s evidence they improve daytime functioning and reduce fatigue.
Some of us are tired for the simplest of reasons, yet unaware of it, says Newton. She sees hundreds of patients in her fatigue clinic in Newcastle, and for many the cause is almost too obvious for them to see. “It’s amazing how many people don’t associate their daytime fatigue with poor night-time sleep,” she says. “Sometimes it’s simply a matter of getting enough sleep. People tend to just carry on doing what they’ve always done and don’t rest properly.
“People are amazed when I ask them to do an activity diary, and then I ask: ‘Well, when actually do you rest?’ And they say: ‘I’m resting here, when I’m on Facebook’. And I have to tell them, sorry, but that’s not resting.
“We’re in a society on a treadmill. We’re all push, push, push. And sometimes that just isn’t sustainable, physically and mentally.”
This is an extract from issue 313 of BBC Focus magazine.
Subscribe and get the full article delivered to your door, or download the BBC Focus app to read it on your smartphone or tablet. Find out more
[This article was originally published in October 2017]
Follow Science Focus onTwitter,Facebook, Instagramand Flipboard

