The Oxford/AstraZeneca coronavirus vaccine is associated with a slightly increased risk of some bleeding disorders, research suggests.
An analysis of people who received a first dose of the AstraZeneca or Pfizer/BioNTech jab revealed a small increased risk of an autoimmune bleeding disorder known as immune thrombocytopenic purpura (ITP) associated with the AstraZeneca vaccine.
The research also suggested there may be evidence of an increased risk of other bleeding and vascular events associated with the vaccine.
“ITP is a condition where the immune system destroys a person's own platelets. Platelets help prevent bleeding. Bleeding symptoms are usually mild and death from ITP is very rare,” said Dr Will Lester, consultant haematologist at University Hospitals Birmingham NHS Foundation Trust, who was not involved in the research.
Researchers said these very small risks are important but rare, and are comparable with those of other jabs, including vaccines against hepatitis B, measles, mumps and rubella, and flu.
Clinical trials have demonstrated the Pfizer and AstraZeneca coronavirus vaccines have been generally well tolerated, although there has been a small number of reports of serious side effects.
The UK’s Medicines and Healthcare products Regulatory Agency (MHRA) received 209 reports of thrombocytopenic and thromboembolic cases – bleeding disorders and blood clot disorders, respectively – after 22 million first doses and 6.8 million second doses of the AZ jab.
Read more about coronavirus vaccines:
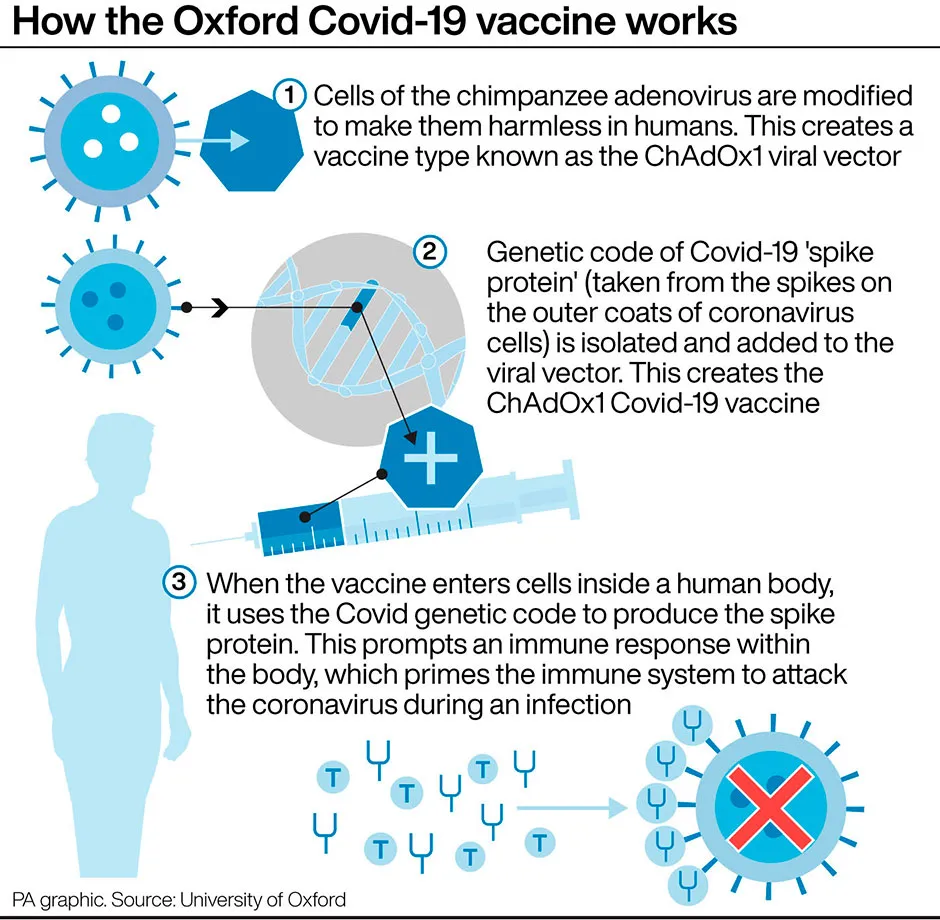
- Oxford/AstraZeneca vaccine turns cells into ‘little factories’ to fight off COVID-19
- COVID booster shots: How do they work and when will we need them?
- Pfizer vaccine approved for children aged 12-15: Everything you need to know
Prof Aziz Sheikh at the University of Edinburgh, and colleagues, examined cases of vaccine-related bleeding and vascular events among 2.53 million adults in Scotland (57 per cent of the adult population aged 18 and older) who received their first doses of vaccines between December and April. The researchers found that for these people, the AZ jab was associated with a slightly increased risk of ITP up to 27 days after vaccination.
The disorder can cause minor bruising in some patients and excessive bleeding and long-term illness in others. It was at an estimated frequency of 1.13 cases per 100,000 first-dose vaccinations.
The analysis also found very small increased risks of other arterial blood clot and bleeding events associated with the jab up to 27 days after vaccination.
However, there was insufficient data to conclude there was an association between the AZ vaccine and cerebral venous sinus thrombosis – a rare condition in which a blood clot forms in the brain.
There was no evidence of an increased risk of the adverse events associated with the Pfizer vaccine.
The researchers stress the findings need to be understood within the context of the clear benefits of the AZ vaccine.
The risk of developing a serious adverse event related to the vaccine is far lower than the risk of serious illness or death caused by coronavirus, particularly for elderly and other vulnerable populations.
Further research involving younger people and to assess responses to second doses of the vaccines is needed.
“The overall message is that, even if the Oxford/AstraZeneca vaccine does have an increased risk of ITP, its benefit outweighs its risk," said Stephen Evans, professor of pharmacoepidemiology at London School of Hygiene & Tropical Medicine, who was also not involved in the research.
“For the majority of people, ITP does not cause serious problems but it is not the case for everyone.”
“Unlike the rare syndrome of vaccine-induced immune thrombocytopenia and thrombosis (VITT) described after vaccination with the AZ and J&J (Johnson & Johnson) COVID vaccines, immune thrombocytopenia (ITP) is generally manageable," said Lester.
The study is published in Nature Medicine.
The findings come after concerns were raised about the AZ vaccine being linked to blood clots.
The Joint Committee on Vaccination and Immunisation (JCVI) said there is an “extremely small risk” of people suffering blood clots after having the jab.
It advised that another vaccine should be offered to under-40s without underlying health conditions where an alternative is available, and as long as it does not cause any substantial delays to the vaccination programme.
Read more about vaccines: