With now over half the UK population having received two coronavirus jabs, the UK's COVID-19 vaccination programme continues at pace.
Ahead of the expected easing of most social distancing restrictions – including a requirement to wear a face mask in most indoor settings – on 19 July, the government is now racing to vaccinate as many possible. Scientists have also highlighted the need for more vaccinations in the face of the highly transmissible Delta variant, which is now the dominant strain of the virus in the UK.
Currently, all people over 18 are eligible for a coronavirus vaccine in England, Wales, Scotland and Northern Ireland. More than 79 million doses have been administered across the four nations, with 34 million people now fully vaccinated.
Officials are confident these high rates of vaccination have weakened the link between case numbers and hospitalisations. Indeed, both rates of hospitalisation and death are lower now than at the end of summer 2020.
On 1 June 2021, the UK reported zero deaths related to COVID within 28 days of a positive test for the first time since the start of the pandemic. However, Health Secretary Sajid Javid has warned that case numbers could reach over 100,000 a day in the coming months, with the country facing a third wave of infections.
Currently, the Pfizer, Moderna, Oxford/Astrazenecaand the one-shot Janssen vaccines are approved for use throughout the UK. They have been shown to be many times more effective than initially predicted – above 90 per cent in some instances. Other vaccines, such as those produced by Novavax and Valneva, have not yet been approved for use.
Although most vaccines have demonstrated a high efficacy rate in trials, medical experts have stressed it is still possible to become infected – and fall seriously ill or worse – from coronavirus if you are fully vaccinated. However, NHS leaders, such head of NHS Providers Chris Hopson, have said it is "incredibly striking" how few hospitalised patients had been given two doses.
Several key questions still remain. Are yet more vaccine types being readied for use in the UK? How exactly do they work? Will they be effective against new coronavirus variants? Will children be vaccinated? And when will we need booster jabs?
Here’s everything you need to know about the coronavirus vaccines.
COVID vaccine UK: what vaccinations are being developed? How effective are they?
Four coronavirus vaccines have been approved for use in the UK after demonstrating promising trial results in protecting people against COVID-19.
- Pfizer-BioNTech (mRNA)– After conducting their final efficacy analysis, the two drug companies announced their vaccine is more than 94 per cent effective in over 65s. The findings were based on a study of 41,000 participants around the globe. The jab has been approved for use in the UK, including for 12-15-year-olds and delivery is ongoing.
- Oxford University-AstraZeneca (viral vector). The vaccine was shown to be, on average, 70 per cent effective in an analysis of phase 3 trial data. While administering two full doses of the vaccine a couple of months apart yielded 62 per cent effectiveness, a half dose followed by a full one later showed to be 90 per cent effective. The jab has been approved for use in the UK and it is currently being administered across the UK, although under-40s are being offered alternatives due a possible link with rare blood clots.
- Moderna (mRNA). In a trial of more than 30,000 Americans, the vaccine showed to be nearly 95 per cent effective. This vaccine has been approved for use in the UK, with the first jabs now being administered.
- Janssen (viral vector). The one-shot vaccine, developed by American manufacture Johnson & Johnson, has been shown to be 66 per cent effective at preventing moderate to severe COVID-19, and has been approved for use in the UK. The government has ordered 20 million doses and it's thought some will be used as booster jabs in the autumn, especially in care home settings.
There are also several other vaccines that are yet to be approved for use in the UK.
- Valneva (inactive whole virus). The vaccine has been trialled on 150 volunteers at testing sites in Birmingham, Bristol, Newcastle and Southampton, with early results showing 90 per cent immune response. Valneva will expand the study to 5,000 people in phase 3 testing.
- Novavax (‘subunit’ or protein adjuvant). The vaccine has been shown to be 89.3 per cent effective in large-scale UK trials. Significantly, it is the first jab shown to be effective against the UK variant of COVID-19 in such a trial. Other trials have shown it is effective against all known variants and – significantly – because it's based on 'older' vaccine technology, it could be easier to produce quickly and at scale. The government has ordered 60 million doses of the jab, which will be produced in Stockton-on-Tees, England.
- Gamaleya / Sputnik V (viral vector). In a press release, the Gamaleya National Center of Epidemiology and Microbiology in Moscow claimed a large-scale Russian study saw 92 per cent efficacy for its vaccine. However, other scientists have voiced concerns this claim is based on too few cases. Although the vaccine was trialled on 18,000 people, the efficacy claim has been based on an analysis of only 39 individuals to test positive with coronavirus.
- Sinopharm-Beijing (inactive whole virus). This vaccine, developed by a state-owned company in China, was the first created by a non-Western country to get WHO approval. Millions of doses have been administered in China and it's been exported to more than 50 countries globally. Efficacy at preventing symptomatic cases and hospitalisation is said to be 79 per cent.
- Coronavac / Sinovac (inactive whole virus). Another vaccine produced in China, this also works by injecting inactivated virus into the body of the person receiving it. Different trials have reported markedly different results in terms of its efficacy but nothing short of 65 per cent effective.
- Covaxin / Bharat Biotech (inactive whole virus). One of India's most widely used vaccines, this was found to be 81 per cent effective in preliminary stage-three trials. Bharat Biotech, the firm behind Covaxin, is aiming to produce 700 million doses by the end of the year.
- CanSino (viral vector). This Chinese vaccine, developed by Cansino Biologics, was shown to be 65 per cent effective in tests. It's a one-shot vaccine, although the company has also trialled an inhaled version of it.
- Sinopharm-Wuhan (inactive whole virus). Another vaccine developed by China's Sinopharm, this one was shown to have 72 per cent effectiveness against symptomatic disease in stage-three trials.
- EpiVacCorona/ Vector Institute (peptide vaccine). Like Russia's first vaccine, Sputnik V, this one was rolled out in the country before Phase III clinical trial results were announced. However, it has attracted criticism from international experts over its efficacy, which intensified when an independent trial found that as little as 75 per cent of participants produced any antibodies.
- Abdala (protein subunit vaccine). Produced in Cuba, this vaccine has undergone Phase III trials but as yet, no results have been published. In trials, participants took three doses.
- Soberana02 (conjugate vaccine). Cuba's other vaccine works by combining a weak antigen with a strong antigen to produce an immune response in an individual. Phase III results are not yet published but Cuba nevertheless intends to produce 100 million doses.
- QazVac (inactive whole virus). Developed in Kazakhstan, this vaccine is awaiting results from Phase III trials but officials have said that it's effectiveness is high and that no side effects are reported. It requires two doses, three weeks apart.
- HayatVax / Sinopharm (inactive whole virus). This is essentially the same vaccine as those developed by Sinopharm in China (see above), but it is produced in the UAE in partnership with local biotech firms Group 42 and Julphar.
Many other companies are also developing vaccines, with major trial results yet to be announced.
How do the coronavirus vaccines work?
Although the inner workings of each complex vaccine differ, they essentially all use the same strategy to protect us from coronavirus: fooling our bodies into thinking we’ve been infected.
By doing this, it allows our immune systems to build a memory of COVID-19, meaning it is better prepared to fight against it in future.
Here are the four main types of COVID-19 vaccine:
Viral vector vaccines
This is the type of vaccine created by Oxford University-AstraZeneca. It works by injecting your body with a genetically altered common cold virus from chimpanzees (what's called an adenovirus). This lab-modified virus can’t replicate in the body or harm it, but does carry the genetic instructions used to create the protein spikes or ‘crowns’ that can be found on the coronavirus. These spikes aren’t harmful in themselves – they’re simply what the coronavirus uses to latch onto cells.
After injection, the vaccine virus enters a human cell. There it uses the cell’s nucleus to ‘photocopy’ the genetic instructions of how to make the coronavirus protein spikes. This causes the cell to produce its own spikes, prompting the body’s white blood cells to attack it. This means that if confronted by a real COVID-19 outbreak, your immune system can recognise these spikes and has a tried and tested battle plan.
Read more about viral vector vaccines:
mRNA vaccines
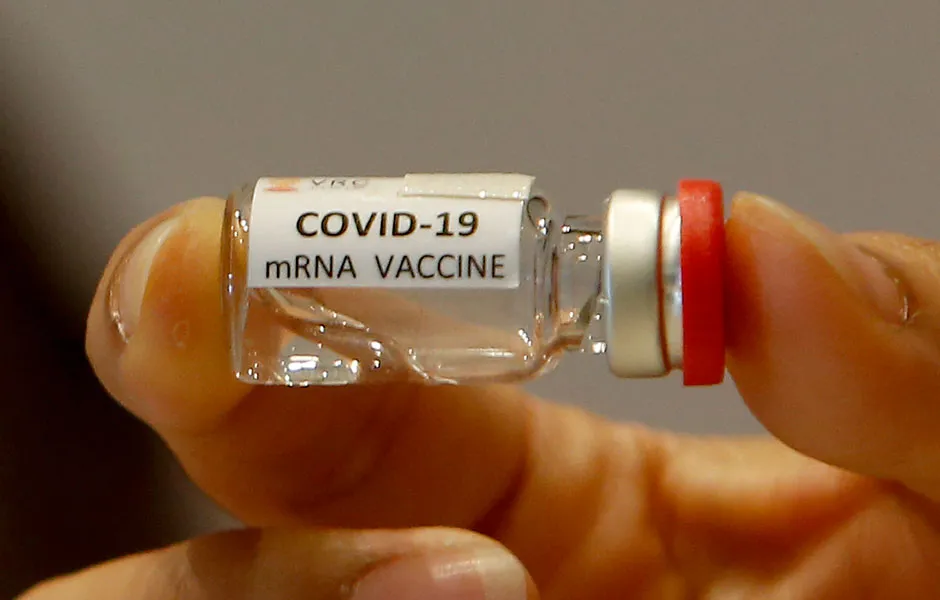
The type of vaccine developed by Pfizer, an mRNA works in a similar way to a viral vector vaccine. Both are designed to prompt some of the body’s cells to produce coronavirus spikes – crowns that provoke an immune response.
However, the mRNA vaccine somewhat streamlines the process. Instead of forcing cells to ‘photocopy’ genetic instructions, the vaccine is a collection of instructions that enters a few of your cells.
These fragile genetic codes need to be stored at very low temperatures (the Pfizer vaccine requires -70°C). Viral vector vaccines, however, can be stored at regular fridge temperature.
Protein adjuvant vaccines
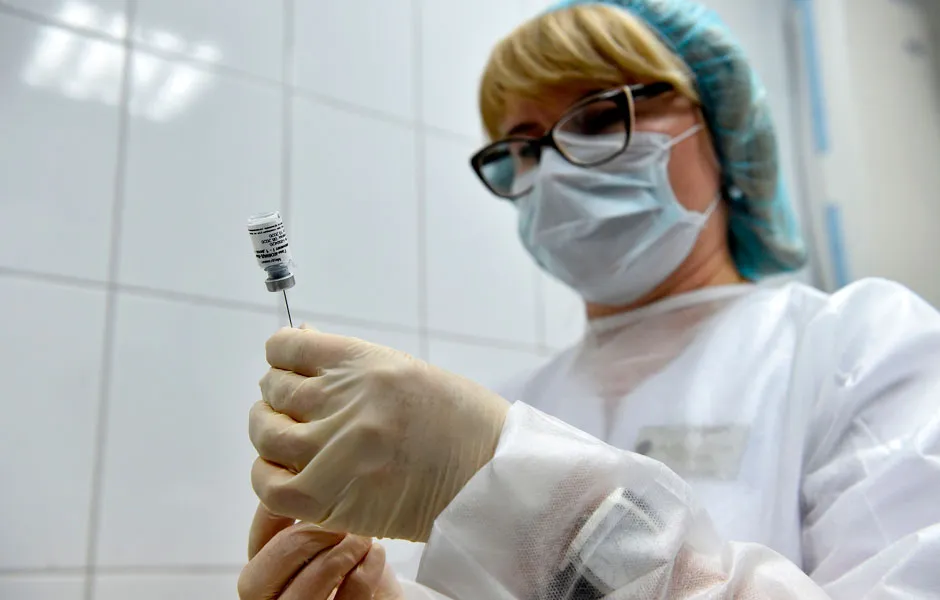
Like several other vaccines, the protein adjuvant approach relies on teaching your immune system to recognise SARS-CoV-2’s protein spikes. However, while the mRNA and viral vector vaccines work by making some of your own cells produce these crowns, this vaccine directly inserts protein spikes into the body.
“This involves purifying just one component of the virus away from everything else,” explains Dr David Matthews, virologist from the University of Bristol. “It’s essentially growing huge amounts of cells that are expressing spikes. And then purifying the spike away from every other part of the virus.”
Inactivated whole virus vaccines

As the name suggests, this vaccine inserts a dead or inactive version of the SARS-CoV-2 virus into the body, triggering an immune response.
While simple in theory, these vaccines are incredibly difficult to produce. “The biggest problem you have here is manufacturing it,” says Matthews.
“You’ve got to make a lot of it. To make a huge amount of a highly dangerous virus and then kill it – making sure it’s definitely dead – is a massive task.”
Peptide vaccines
This type of vaccine uses short chains of amino acids to do the same thing as many other vaccines: teach an organism how to attack a pathogen. "This would use a small part of a protein – typically a part you are very sure the immune system recognises – and then would successfully attack a genuinely infected cell," says Matthews.
However, there are limitations: Russia's EpiVacCorona, a peptide vaccine, has been criticised after independent studies found that it did not produce an immune response in all who received it.
Do the coronavirus vaccines have any side effects?
No drug, including paracetamol, is 100 per cent safe from extremely rare allergic reactions. Regulators in the UK and the EU have been investigating a link between the Oxford-AstraZeneca jab and rare but potentially fatal blood clots (see 'Is the Oxford vaccine safe?' below), as well as other vaccine side effects in those from different manufacturers.
A COVID-19 vaccine will only be approved for use on the general population once it has met robust standards on safety through extensive clinical trials. It’s down to the UK’s medicine regulator MHRA (Medicines and Healthcare products Regulatory Agency) to authorise any vaccine, which it will analyse over several weeks.
Read more about coronavirus vaccines:
- Coronavirus vaccine: Is it safe?
- Should we infect people with COVID-19 for vaccine research?
- COVID-19: Who should get a vaccine first?
Is there any serious worry that a vaccine could cause hidden long-term effects? “That is a potential problem with any drug you could imagine. But the technology to build many of these vaccines, such as the Oxford one, has been used before. It’s not like we’re guessing – we know exactly what we’re doing,” says Matthews.
However, while trials are good at finding common side effects to new vaccines, rare effects will only become apparent when they are given to huge numbers of people.
“You also really have to ask: what are the long-term effects of catching coronavirus? Do you want to take a risk with a virus that can kill at all ages? Or do you want to take a vaccine for which we are as confident as we can be that there are no fatality risks?”
Is the Oxford vaccine safe?
A number of European countries suspended, then resumed, use of the Oxford-AstraZeneca vaccine in recent months. Prompted by a small number of blood clots in people who had received the vaccine, Denmark was the first country to pause its use of the vaccine. It was followed by Norway, Iceland, Germany, France, Ireland, Italy, Cyprus, Spain, Latvia and Sweden. Other countries have suspended use of specific batches.
Investigations by regulators in the UK and EU have concluded that, while it's not conclusive, there is mounting evidence of a link between the vaccine and extremely rare blood clots.
It has prompted the UK to change course on its vaccination programme, with under-40s now being offered an alternative to the Oxford-AstraZeneca jab. The European Medicines Agency, meanwhile, doesn't recommend restricting the vaccine, although it has said that recipients should be warned of potential side effects, just as they would with other medicines.
Both regulators have stressed that the vaccine is safe for the majority of people, and that the benefits outweigh the risks. It's estimated that four in a million people can experience the side effects.
Up to the end of April, there had been 209 cases of blood clots in the UK and 41 deaths. That's against more than 20m vaccines administered. Women seem to be more at risk, and there is also a slightly higher risk in young people. However, the risk of developing a blood clot across all ages is higher if you develop COVID-19.
The UK's regulator, the MHRA, as well as the Joint Committee on Vaccines and Immunisations say that another factor in the decision to offer under-40s an alternative vaccine is because, at that age group, the risk from COVID-19 itself is not very high.
Will the vaccines work against the new emerging variants?
Several major coronavirus variants have identified in recent weeks and months. Originally known by their association with the country or region where they first developed, the World Health Organisation later These include:
- The UK coronavirus variant (B.1.1.7 / Alpha variant). A study has shown the Pfizer vaccine appears to protect against this variant, however, the results have not yet been peer-reviewed. Plus, the yet-to-be-approved Novavax vaccine has shown an 89 per cent efficacy in large-scale UK trials.
- The South Africa coronavirus variant (B.1.351 / Beta variant). A study from Pfizer has indicated their vaccine is effective against this strain. However, these findings have not yet been peer-reviewed. The Novavax vaccine is also believed to highly effective against it.
- The Brazil coronavirus variant (P.1 / Gamma variant).No large scale trials have yet emerged examining vaccine efficacy against the this variant of the virus, but a small study has indicated the Pfizer vaccine protects against the UK, Brazil and South Africa strains.
- The Indian coronavirus variant (B.1.617.2 / Delta variant). Initial studies have found that the Pfizer, AstraZeneca and Novavax vaccines are effective against this highly transmissible variant after two doses. However, the jabs are only 33 per cent effective three weeks after a single dose. That compares to 50 per cent effectiveness against the UK variant. The variant is believed to be 40 per cent more transmissible than the Alpha variant.
As long as COVID-19 continues to circulate, the risk of new variants will not go away. Each infection gives the virus another opportunity to mutate, and the larger-scale fears are of variants that evade immune responses or are more transmissible or deadlier to a greater number of people.
In that scenario, new variants could potentially re-infect people who have either had the virus or a vaccine. This would necessitate updated vaccines and booster jabs similar to those for seasonal flu. Several world leaders, including Boris Johnson, are pushing to vaccinate all adults globally, before vaccinating teenagers and children, in a bid to lower the risk from new variants.
However, the single best strategy to stop the spread of new variants is to drive infection rates as low as possible, thereby limiting the opportunities for mutations.
Read more:
When will the coronavirus vaccines be rolled out?
Many of the approved coronavirus vaccines are currently being administered across the UK.
The Pfizer vaccine has been approved for use in the UK. On 2 December, the government announced: “The vaccine will be made available across the UK from next week." The first person to receive the coronavirus vaccine was 90-year-old Margaret Keenan, on 8 December.
Almost a month after the rollout of the vaccine developed by Pfizer, the jab from the University of Oxford and AstraZeneca was approved and in January 2021 began being administered in hospitals and GPs across England.
After being approved on 7 January, the first doses of the Moderna vaccine were given in early April.
The Janssen vaccine was approved at the end of May with the first doses expected towards the end of the summer.
Will children be given a coronavirus vaccine?
This is the subject of quite intense debate, although the UK regulator has approved the use of the Pfizer vaccine in adolescents aged 12-15 and some countries, including the US, have begun administering vaccines to this age group. The regulator is currently reviewing evidence on the need to vaccinate younger children here.
In the UK, COVID-19 is thought to be spreading faster in children than in adults, but that's not necessarily a reason to give them doses. If children are not generally vulnerable to the virus, then it's argued that doses are put to better use in the arms of vulnerable adults in other countries. Beyond the ethics of such a decision, this might also lower the risk of new, vaccine-proof variants emerging around the world.
However, if children are spending a lot of time with vulnerable adults in, for example, multi-generational households, then vaccinating them could offer their vulnerable relatives an extra layer of protection.
How are the vaccines being distributed?
Per July 2021, there were more than 2,000 vaccination centres across the UK, a mix of large-scale mass vaccination centres and smaller pharmacy services. 99 per cent of the population are within 10 miles of a vaccine service.
As the Pfizer-BioNTech and Moderna vaccines must be stored at low temperatures, they are unlikely to be taken directly to care homes. However, some governments have now taken the decision to store the vaccine in regular refrigerators. The Oxford and Janssen vaccines can be stored at fridge temperature.
The government is also organising roving teams of healthcare workers who can visit care homes and housebound people.

The vaccine will likely be administered via injection, although there is some hope it can be distributed through a nasal spray. A team at Swansea University are working on a prototype for a COVID-19 vaccine 'smart patch'.
“There are certainly good arguments for delivering a vaccine’s payload directly to the upper respiratory tract like modern flu vaccines,” says Matthews.
“That will raise an immune response at what's called the mucosal surfaces – the surfaces of the nose, mouth and the back of the throat. That’s where you really want a strong and effective immune response if you're going to beat off a respiratory virus.
“However, at the moment, inducing good immunity by such a spray is less understood than an injection.”
In what order will we get the coronavirus vaccine?
Currently, all people aged 18 or over can book a jab in England, Wales, Scotland and Northern. This can be done by accessing the NHS vaccine online booking system for each respective country,or by calling 119.
The government prioritised the most vulnerable people, with the Joint Committee on Vaccination and Immunisation (JCVI) has recommended a priority order, based on who is at the highest risk of death. By early June, people aged 25-29 were being called for their first jabs, with the government aiming to have all adults receiving at least one vaccination by the end of July.
Public appeals to come forward for vaccine appointments also intensified as clusters of the Delta variant grew in a number of towns and cities.
The JCVI order is:
- Older adults in a care home and care home workers
- All those aged 80 and over and health and social care workers, though they may move up the list
- Anyone 75 and over
- People aged 70 and over
- All those aged 65 and over
- High-risk adults under 65
- Moderate-risk adults under 65
- All those aged 60 and over
- All those 55 and over
- All those aged 50 and over
- The rest of the population, with priority yet to be determined.
However, experts have warned that the general public should not get their hopes up that life could return to normal once the high-risk had been vaccinated. Although many social restrictions – including a legal requirement to wear a face-covering in certain indoor areas – are being dropped on July 2019, certain rules remain in place. These include the need to isolate if you are tested positive for coronavirus.
For further analysis, check out our 'Will COVID-19 be over by 2022?' explainer.
Will we need a vaccine booster or third dose?
It's not currently known how long protection lasts from any of the approved vaccines, but most scientists and officials believe that seasonal booster jabs will be required that work in the same way as a seasonal flu jab. In May, the UK government launched a trial looking at seven different booster vaccines. This will assess the impact of a third dose on people's immunity. Thousands of people are involved in the trial, with results expected in September.
Do the coronavirus vaccines protect you from long COVID?
Currently, there is no major study highlighting how well a coronavirus vaccine protects a person from suffering from long COVID.
However, when posed this question at a Downing Street press conference on 5 July, Chris Whitty (Chief Medical Officer for England) said that although the data is currently unclear on this issue, we can be confident that the vaccines offer protection from catching COVID, in itself a protection against long COVID.
Can the vaccines be mixed?
Not currently. If you are given a dose of the Oxford jab, your second dose must also be Oxford. The same goes for the Pfizer coronavirus vaccine.
However, Dr Mary Ramsay, head of immunisations at Public Health England has said, on “extremely rare occasions” the same vaccine is not available, or if there is no record which jab a person received first, a different vaccine may be administered for the second dose.
Yet again, scientists have also said there is likely no harm in receiving two doses of different vaccines and it may even prompt a bigger immune response by having different vaccines.
In fact, a study investigating this issue (known as Com-CoV) appear to show just this. Its study of 850 volunteers found that those who received either Pfizer or AstraZeneca as their first vaccine, with a jab of the other type four weeks after, were highly protected against coronavirus. However, the study also found that those who mixed vaccines were more likely to experience side effects.
Will we get a choice about which vaccine we are given?
As things stand, the vaccines will be rolled out as and when they become available. However, after an investigation into the risks of blood clots with the Oxford-AstraZeneca vaccine, those under 40 will be offered an alternative.
How many coronavirus vaccines have the UK ordered?
The UK government has secured orders for millions of doses of several different vaccines.
These include up to 100 million doses of the AstraZeneca/Oxford University coronavirus vaccine, enough for the majority of the UK’s population of 66.7 million (with each individual needing two doses).
Overall, the UK has secured access to 340 million doses across four separate types of vaccine – adenoviral vaccines, mRNA vaccines, inactivated whole virus vaccines and protein adjuvant vaccines (read more about how each works above).
As of April 2021, these include:
- 60 million doses of the Novavax vaccine
- 20 million doses from Janssen
- 40 million doses of thePfizer/BioNTech vaccine– the first agreement the firms signed with any government
- 100 million doses of a vaccine being developed by Valneva
- 60 million doses of protein adjuvant vaccine from GlaxoSmithKline (GSK) and Sanofi Pasteur
- 17 million doses of the jab on offer from Modernain the US
- 100 million dosesof the Oxford vaccine
Why so many? “What the government has done is order different vaccine classes,” explains Matthews. “It’s that simple.”
Read more:
- How do viruses jump from animals to humans?
- How do viruses make us ill?
- Who really invented vaccinations?
- How are seasonal flu vaccines made?
About our expert Dr David Matthews
Dr David A Matthews is a reader in virology at the University of Bristol, with over 30 years of experience in the subject. His work centres on virus-host cells and he specialises in respiratory viruses. He has also worked on COVID-19 and is collaborating with others to develop new ways of studying viruses that are dangerous to humans in their original host animals.

