Previous COVID-19 infection provides some immunity for at least five months, but people may still carry and transmit the virus, according to a new study.
Experts have warned that a small number of those with immunity may still be able carry the virus in their nose and throat and therefore have a risk of transmitting it to others.
The first report from Public Health England’s (PHE) Siren study found that antibodies from past infection provide 83 per cent protection against reinfection for at least five months.This suggests that people who contracted the disease in the first wave may now be vulnerable to catching it again.
Although reinfections in people with antibodies were rare, the researchers identified 44 potential reinfections among 6,614 participants who showed evidence of previous infection.
Read more about COVID-19:
- Ventilation and viral loads: the key misunderstandings of how coronavirus spreads
- Coronavirus vaccine: Is it safe?
“This study has given us the clearest picture to date of the nature of antibody protection against COVID-19 but it is critical people do not misunderstand these early findings," said Professor Susan Hopkins, senior medical adviser at PHE and the Siren study lead.
“We now know that most of those who have had the virus, and developed antibodies, are protected from reinfection, but this is not total and we do not yet know how long protection lasts. Crucially, we believe people may still be able to pass the virus on.
“This means, even if you believe you already had the disease and are protected, you can be reassured it is highly unlikely you will develop severe infections, but there is still a risk that you could acquire an infection and transmit to others.
“Now, more than ever, it is vital we all stay at home to protect our health service and save lives.”
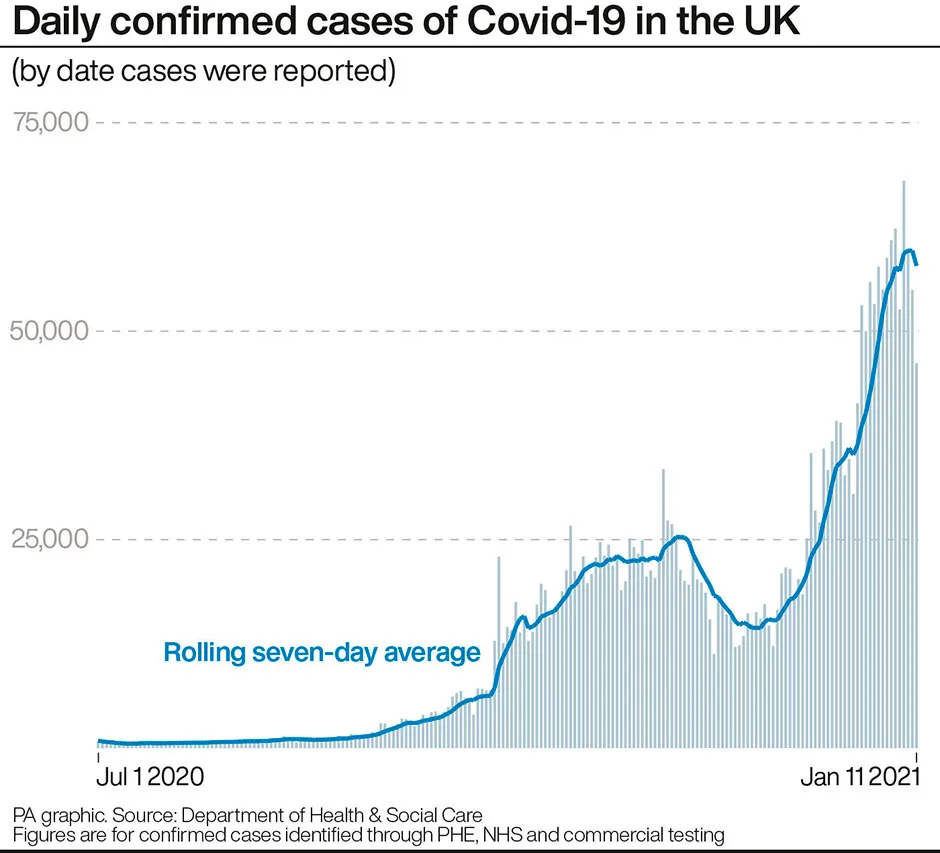
Since June, PHE has been regularly testing tens of thousands of healthcare workers across the UK for new COVID-19 infections as well as the presence of antibodies, which suggest people have been infected before.
The study leaders are clear that this first report provides no evidence towards the antibody or other immune responses from coronavirus vaccines, nor should any conclusions to be drawn on their effectiveness.The study, which has not been peer-reviewed, will consider vaccine responses later this year.
PHE said early evidence from the next stage of the study suggests that some of these individuals carry high levels of the virus and could continue to transmit it to others.
Read the latest coronavirus news:
- COVID-19 and the brain: Does the virus cause psychiatric problems?
- Pfizer vaccine may protect against new strains of coronavirus
- COVID-19 vaccine 'smart patch' uses microneedles to deliver immunity
Prof Hopkins said she can be confident that five to six months after their first infection, the vast majority of people with a previous infection are protected from severe disease and are protected from symptomatic infection.
“It is good that it’s protecting people, but it’s not 100 per cent protective, and therefore people still need to follow the rules, until we know more about this, on the durability of the response, and also understand better why some of these individuals have not responded, or is this particular to a certain group,” Prof Hopkins added.
“Overall I think this is good news, it allows people to feel that their prior infection will protect them from future infections, but at the same time, it is not complete protection, and therefore they still need to be careful when they’re out and about.”
“I am strongly encouraged that people have immunity that is lasting much more than the few months that was speculated before the summer,” Prof Hopkins said.
Coronavirus vaccines: Is it safe to mix them?
At the moment, scientists have no reason to think a combination of vaccine doses from different manufacturers would cause harm. And, to confirm this, the UK’s Vaccine Taskforce has announced trials examining the interchangeability of the COVID-19 vaccines.
The very fact these human trials have been greenlit is a good indication, says Dr David Matthews, virologist at the University of Bristol.
“You wouldn’t even be able to start them if a lot of people thought they’d be a problem,” he explains. “An ethics body, hospitals and other scientists will only go ahead with these trials if everyone is very confident that nothing horrible is going to happen.
“And if it turns out down the road there’s a problem then we’re going have to do a lot of science to work out why there’s an issue. But everything we know so far about vaccines and the way vaccines work says this shouldn’t be a problem. It’s not like such vaccines have been dropped down from a spaceship – we’ve had a long time to study them.”