According to much of what we see on social media, in magazines and on TV, the fat on our bodies is something we need to either fight constantly with exercise and diet, or stop worrying about and celebrate. But in reality, our fat is far more than just a symbol of how healthy our lifestyle is, or of how body confident we may be.
Fat is one of the most important elements of our diet, and the fatty tissue beneath our skin plays a part in keeping us alive and healthy. In chemical terms, fats are long, chain-like molecules that have many roles across all forms of life on Earth.
Among their many useful properties, they are an excellent way to store energy, and many organisms convert energy from the food they eat into reserves of fat – from the vegetable oils found in the seeds and fruits of plants, to the inches-thick layer of blubber beneath the skin of large marine mammals.
It is only in recent decades, as an abundance of energy-rich food has caused an epidemic of obesity worldwide, that this vital component of our diet has become so problematic. Whenwe store too much fat, it causes the vital functions of our fatty tissue to start to fail, leading to many different health issues, from diabetes to stroke to fatty liver disease.
For most of human history, though, our ancestors were more preoccupied with dying from malnutrition and hunger than with looking toned and svelte, and our body fat was the energy store that saved people when food was scarce. In many non-Western cultures, animal fat remains something of a luxury food item, or even a delicacy.
Read more about fat:
- Thought experiment: How fat do you have to be to stop a bullet?
- How long could you live off body fat alone?
- Can you target belly fat with pills and exercise, like the ads say?
When we talk about body fat, we’re actually talking about the specialised cells, known as ‘adipocytes’, which store fat in various places in our bodies. Each cell holds its own droplet of liquid fat and is capable of swelling to accommodate more fat, or shrinking and releasing it as necessary. Together, these fat cells form ‘adipose tissue’, which is found in deposits just below the skin or deep in the spaces between other organs.
As well as storing energy, these fat deposits help to insulate us from the cold and cushion impacts on our joints, the soles of our feet, our palms and our bums – people with no adipose tissue find it hard to sit on a chair for more than a few minutes.
Fatty tissue is part of the complex connective tissue that keeps our organs in place, and is key to building the contours of our faces that make us recognisable. Perhaps more importantly, adipose tissue can be thought of as the body’s energy budget-holder, helping ensure different parts of the body have what they need, but always looking to store and save for hard times ahead.
In fact, adipose tissue plays such an important role in tracking our energy requirements and coordinating our metabolism that scientists increasingly think of it as an organ of the body in its own right, albeit one that is distributed throughout the body.
“We need our adipose organ to buffer our normal fluctuations of caloric intake and expenditure,” says Prof Stephen O’Rahilly, a co-director of the University of Cambridge’s Institute of Metabolic Science.
“We don’t drip-feed ourselves calories to match exactly the amount we need on a minute-to-minute basis, and after each meal, any calories in excess of what we immediately need are safely stored away in adipocytes.
“If, for any reason, we don’t have this storage space, then that excess energy in the form of fat is redirected to our bloodstream, liver, muscle or pancreas. None of these are designed to store fat, and all of them are readily damaged by trying to do so.”
Far from consisting merely of unsightly lard deposits, the adipose organ has a rich supply of blood vessels and nerves, and produces a variety of hormones and signalling molecules. Not only does the adipose tissue release energy when needed, it also sends information to the brain about the state of our calorie stores, influencing our digestion, appetite and behaviour.
“There is growing evidence that how well – or badly – our adipose organ performs these functions is one of the major determinants of whether, in the face of an excess of calorie ingestion, we develop diabetes, heart attacks, fatty liver disease and so on, or whether we remain overweight but basically healthy,” says O’Rahilly.
There are two main types of fat in our bodies: white and brown. White fat (WAT, or white adipose tissue) is all about storage. Under a microscope, a white fat cell looks like a normal cell with a big glob of fat in the middle.
Brown fat (or BAT) is all about heat generation. Brown fat cells look more like normal cells, with smaller droplets of fat dispersed among their components. But they are packed with mitochondria, the bean-shaped energy factories that convert chemicals into the power that drives our metabolism, movement and body heat, giving them a brown appearance.
So-called ‘beige’ fat cells are somewhere between the two.
There are many dietary and genetic factors that can cause people to be prone to weight gain, but one of them may be a genetic disposition to developing more white fat and less brown fat. Studies have shown that people with high levels of brown fat are less likely to develop the cardiovascular and metabolic disorders associated with obesity, such as heart disease and diabetes.
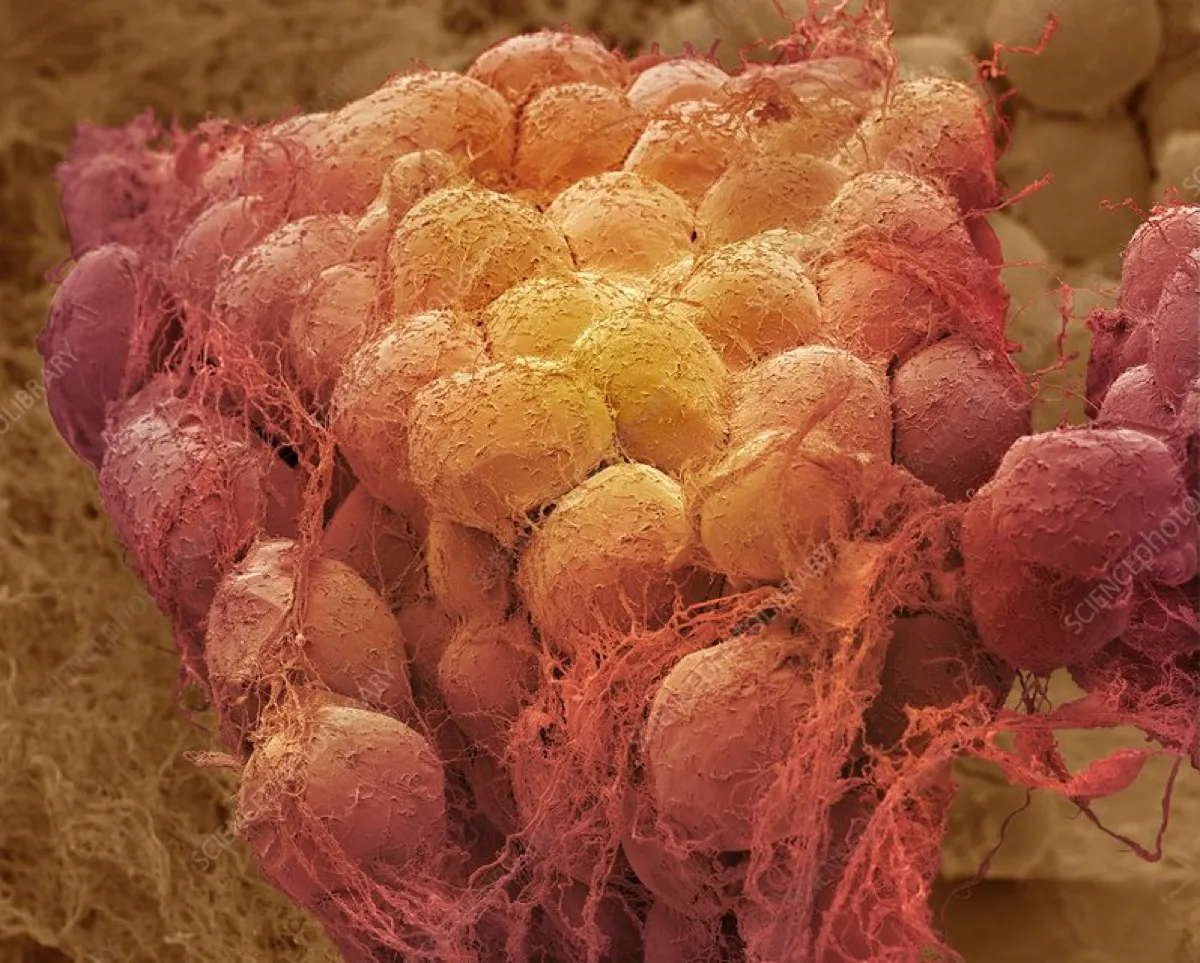
Strangely, white adipose tissue also acts as a kind of reservoir for the special immune cells that help us remember and fight past infections. So you can think of your fat as a kind of wobbly living bank that stores calories, heat and even memories of past infections, all of which can be drawn on when required. Fatty tissue is also central to the development of the specialist milk-producing glands that feed the babies and young of female mammals after pregnancy.
Interestingly, the number of fat cells in your body does not change in adult life, even when your weight fluctuates. We can grow more fat cells during childhood, and white fat cells may swell with more fat when there is more fat to store – and may even turn brown if a person is subjected to cold for a long period – but it is impossible to rid your body of adipose cells and tissue, no matter how much you diet or exercise.
When fatty tissue is physically removed from the body during cosmetic procedures like liposuction, the body compensates for the loss and fat levels soon return to normal, regardless of what patients consume. The lost tissue may even return to the abdomen area or to the spaces between the organs instead of where it was removed from – so while your bum may look great, you suddenly find yourself with a bigger belly than before and poorer overall health.
Some bodybuilders claim to have reduced their body fat to less than 1 per cent of their total weight, but most physiologists believe it is impossible to reduce body fat to such levels: even the most ‘shredded’ or toned athletes will have 2 to 3 per cent body fat.
According to bodybuilding folklore, when Austrian-born muscleman Andreas Münzer died in 1996 his autopsy supposedly revealed he had reduced his body fat percentage to zero. But while he did indeed have a freakishly muscular body, it’s unlikely he was anywhere near zero: he actually died from the stress put on his heart and liver by years of over-exercise and steroid abuse.
Despite scientists’ growing understanding of the importance of fat, high-protein and extremely low-fat diets are still all the rage as people obsess over shedding fat at all costs. But ultra-low fat diets, where fewer than 10 per cent of a person’s calories come from fat, are not very healthy in the long term. Some types of fat are essential to help us absorb vitamins and minerals, and when the amount of fat in our diet is far too low, it can make us seriously ill.
The 2007 filmInto The Wildportrays the last days of Christopher McCandless, a student who died in the Alaskan wilderness after cutting himself off from the outside world and ending up trying to survive on just rabbits and berries.

Rabbit meat, although high in protein, has extremely little fat, and McCandless is thought to have developed an acute illness known as ‘rabbit malnutrition’, where the body uses more energy breaking down the protein in meat than it gets from it. Also known as ‘protein poisoning’ or ‘fat-hunger’, the problem affects those living in cold, harsh conditions, where lean animals like birds, rabbits or rodents can be the only food source. Without a source of fat or more energy-rich food, the more the person eats, the more they starve.
Several extremely rare diseases can cause humans to lose more fat than is healthy, or even to be born with no fat at all. With fat having such a central role to play in regulating our energy use and metabolism, these are serious illnesses with a range of long-term health effects. Babies that are born with no body fat whatsoever look alarmingly muscular and veiny, have trouble staying warm, and quickly develop a suite of serious metabolic conditions such as diabetes.
Of course, an excess of fat is not good for us either. An excessive amount of white fat is associated with many health problems, from cardiovascular disease to cancer.
Obesity is arguably the defining health issue of our time: our bodies have evolved to store fat whenever we come across it, and many of us now live in a world where fatty food is not just plentiful but hard to avoid. At the same time, we lead lives that involve far less physical activity than the lives of generations before us.
When we ingest more calories than we need, our body still stores the excess energy as fat to protect us in the lean times ahead. When those lean times don’t come, our bodies just keep storing more and more fat.
On a cellular level, when white fat cells become too large they start to die, attracting the attention of our immune system, and in particular, a type of immune cell known as a macrophage. The macrophages surround the enlarged fat cell and start to release chemicals into the blood that cause inflammation and stress.
These chemicals eventually play a role in the body becoming less responsive to insulin, the hormone that regulates blood sugar, which leads to diabetes. Fatty substances like cholesterol enter the bloodstream, creating a build-up of fattydeposits in places like the heart, which can lead to cardiovascular conditions such as high blood pressure, stroke and heart attacks. The chronic inflammation caused by over-enlarged fat cells is also thought to increase the risks of some cancers.
To make matters worse, much of our food is packed with saturated fats, which are more likely to exacerbate these problems than unsaturated fats.
Read more about diet:
- Dr Michael Mosley: The Mediterranean diet is great for your gut (even if it makes you fart)
- Can you feed your brain?
- Is there a physical limit to how much food you can eat in one sitting?
Surprisingly, some scientists are beginning to explore how our own fat can, with a little help, actually help us to lose weight. Prof Yu-Hua Tseng, from Harvard University’s Joslin Diabetes Centre, is one of many scientists exploring whether obesity and weight gain can be reversed by activating a person’s brown fat, therefore burning away their fat deposits as heat.
“The bodies of obese people have too much white adipose tissue, and often too little brown,” she says. “The idea of converting the white tissue into brown is a very attractive approach.”
There are a number of ways to do this that could become potential obesity treatments, says Tseng. Some scientists are looking at whether white fat cells can be genetically modified to express the proteins that allow brown fat cells to generate heat from fat, essentially ‘browning’ the white fat so it burns fat rather than storing it. Others are looking at ways to stimulate brown cells to be more active: either by mimicking the body’s own molecules that stimulate brown fat to produce heat, or simply by making people cold.
This may sound even worse than going on a diet, but Tseng stresses that it does not take extreme cold to activate your brown fat. “There are studies looking at so-called mild cold exposure,” she says. “It’s not like freezing cold, it’s more like temperatures of around 55°F [12°C].”
Before you turn the air-con right up or run a cold bath, though, Tseng warns that these treatments are still at the proof-of-concept stage, and a long way off being approved for therapeutic use. Eating a balanced diet in moderation and takingplenty of exercise is still the best way to retain a healthy amount of adipose tissue.
Now we know that our fat is such a vital part of our bodies, perhaps it’s time we built a more sensible relationship with it – one that is based neither on impossible diets and shame, nor on denial of the deadly reality of obesity. Just like our skin, our teeth or our heart, our body fat should be something we want to take care of and keep healthy. If our fat is healthy, we are healthy.

Breaking down the fat myths
Cholesterol = bad
Some is. There are two types of cholesterol: low-density lipoprotein cholesterol (LDL) is the ‘bad’ type that hardens the arteries, but
high-density lipoprotein cholesterol (HDL) will return excess LDL to the liver for processing. Saturated and trans fats boost LDLand lower HDL, while healthier fatsdo the opposite. But beware of claims that so-called superfoods can lower your LDL. The best way to do that is simply to avoid eating too much saturated fat.
Olive oil = good health
True. Many studies have shown that ‘Mediterranean’ diets, high in olive oil, can benefit people’s health and longevity, probably because olive oil contains a high proportion of mono-unsaturated fats, which are very good at lowering LDL cholesterol. But olive oil contains lots of calories – so while it’s the healthiest oil to use, don’t go too mad on the dressing.
Fat = high cholesterol
Not always. Saturated fats, found in meats, cheeses and butter, boost cholesterol in your bloodstream, increasing your chance of stroke and heart disease. So-called trans fats are even worse: these highly processed fats raise cholesterol, make the blood more likely to clot, and cause inflammation. But unsaturated fats from oils, vegetables, fish and nuts actually help reduce cholesterol levels.
High BMI = poor health
It’s complex. Body mass index, or BMI, is a quick but crude way to assess if a person is overweight, based on their height/weight ratio. But it doesn’t really tell you how much excess fat you have: people with lots of muscle, or large, dense bones can have high BMIs and be perfectly healthy. Only a full-body X-ray can provide detailed information on fat levels, both under the skin and around the organs.
- This article first appeared in issue 381 of BBC Science Focus – find out how to subscribe here